Winback tecartherapy accelerates your results in rehabilitation.
Discover our range of tecar therapy devices
It adapts to all your known techniques, bringing efficiency, speed and comfort to your treatments.
Discover the latest range of tecar therapy devices
It adapts to all your known techniques, bringing efficiency, speed and comfort to your treatments.
Multifrequency Winback: your all-in-one solution
High frequency TECAR: metabolic action
Medium frequency Hi-EMS: muscle recruitment
Low frequency Hi-TENS: pain relief
In 10 years, Winback has been able to adapt to the needs of
therapists to develop technologies, techniques and approaches together, techniques and approaches.
Today, Winback has become a worldwide reference
in the world of rehabilitation, high level sports, women's well-being and animal health.
Together, let's Winback!
Discover the studies on tecartherapy
Winback was founded in 2013 to do something no one else had ever done before. We started with the goal of bringing clinical assessment, physical therapy, and manual therapy together in the same treatment.
Combining each therapist’s unique expertise with Winback’s innovative, entirely new technologies in TECAR, Hi-TENS, CRYO and COMPRESSION is creating a new era in therapy and new possibilities for patients and therapists alike.
Therapists provide enhanced treatments with faster recovery times and lasting results. Patients receive an experience that is more delicate gentle and non-invasive. Winback equipment meets a wide range of patient and therapist needs. From basic operation to multiple-layered therapy strategies, our emphasis on training, education, and continued support makes experiencing the full potential of Winback equipment a priority.
To all the physiotherapists, chiropractors, athletic trainers, massage therapists and osteopaths seeking better results for patients and your practice— we’re moving healing and body enhancement forward.
Join the Winback winning spirit!








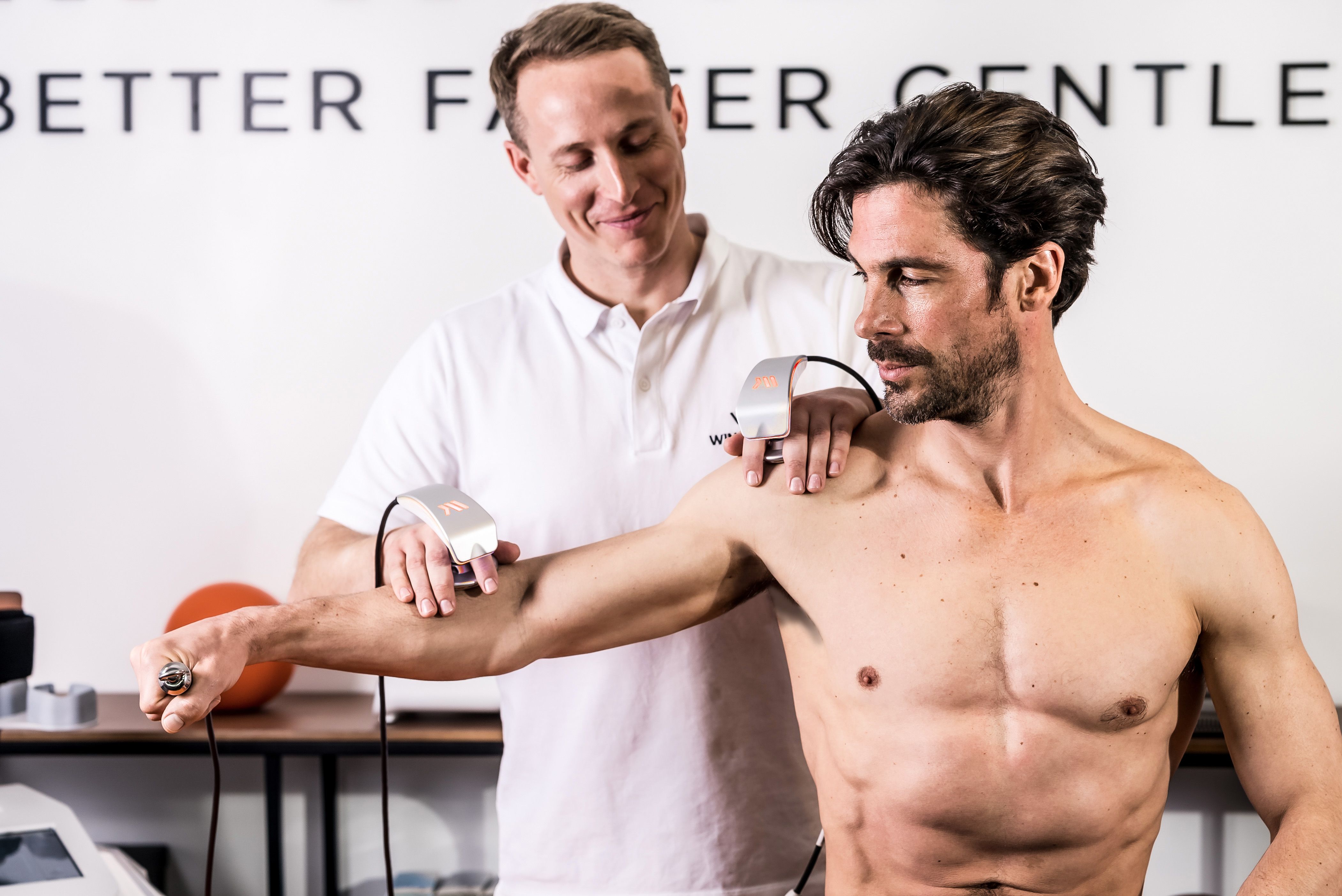




























Endorsed by top-ranking hospitals, clinicians, professional sports organizations, and athletes.
See more testimonials
"Winback helps me to keep a smile on everybody's face...because it works! I did not believe in it at the beggining, until I tested it on myself and then I became a full believer and now we have 2 devices. Winback is so tangible, you can see the results in a 15 minute treatments!"
Doctor and owner of Kessler Family Wellness
"I had to treat a recurrence of adductor tendinopathy in the emergency room two days before a race. The first occurrence of this tendinopathy had been treated over several weeks, making the athlete very sceptical and especially worried about her participation in the week's events. Finally, the beneficial effects were felt from the second session and the athlete was able to participate in the events without functional discomfort.
The Winback was renamed the "magic machine" for the occasion. In contrast to other devices, the Winback tecar therapy does not depend on the rehabilitation act but is performed simultaneously. As I work mainly with my hands, I really liked this approach."
Physiotherapist at the National Ski and Snowboard Centre in Albertville, France
“Winback BACK1 helps me to augment my manual therapy especially for pain diagnosis such as pelvic floor dysfunctions to give more tissue mobility and a better patients tolerance. My patients actually love it and ask for more because they have got a lot of relief after several days.”
Doctor of Physical Therapy, Director Pelvic Health Physical Therapy Residency – Johns Hopkins Hospital, Baltimore, MD, USA
“Sometimes the results are almost instant. The client can feel the heat and of course the penetration of the device and they feel that they’re getting a very good treatment, as well as seeing more movement, less pain, reduction in the scar in terms of the pulling and the tightness, and also the appearance of the scar as well”
Owner of HLP Therapy and Positive C Section. Scar Specialist and Womens Health Physiotherapist, UK
"Llevo 7 años utilizando el BACK3 y me he pasado al BACK4: es una revolución. Ahorra tiempo, es más eficaz, es un aparato muy bien pensado para nosotros y muy apreciado por los pacientes. Bravo Winback!"
Physiotherapist, Kin&Plus Center, Frameries, Belgium
"In 38 years of physiotherapy practice, this is the first device that has fascinated me and imposed itself on my daily practice, giving a breathtaking satisfaction and calling for reflection and manual dexterity. This is a change from the ready-made recipes of the physio devices that turn practitioners into "button-pushers"! What is very appreciable, in addition, is that one finds oneself communicating with a community of competent and sympathetic colleagues."
Physiotherapist, Tunisia
“One of the main things I found is I could treat people without causing pain, and that was such a huge jump forward. I can improve recoveries and get them either back to sport or back to work quicker.”
Clinical Director at GT Physiotherapy, Bridgwater, UK
"The Winback technology intervenes at the cutaneous level, which makes it possible to restore vascularity and to re-soften a very indurated or burnt skin, after radiotherapy for example.
Patients confess that Winback came about after a difficult period, the arm swells and scars appear, necessarily the body is questioned and the future put aside. But with Winback, the patients have access to a real reappropriation of their body. They regain mobility and an image in which they recognize themselves.
Winback in 3 words: Efficiency, Comfort and Performance."
Physiotherapist, France
"I had a patient who fell on a motorbike over a year ago. He had burns on his hand. In 6 sessions of 5 to 10 minutes, the adhesions disappeared."
Physiotherapist, France
“The things that sold me on Winback in that very first week of having the opportunity to use it were how perfectly well it dovetailed with the way I treat, how quickly patients responded to the treatments and how much the patients seemed to value the addition of this cutting edge technology.”
Doctor of Physical Therapy specializing in Pain Management and Orthopedics, USA
"I was introduced to Winback TECAR by a sportsman who asked me to use it. I tested several brands before making my choice. What I liked was its modularity, through all its accessories, but also the fact that the current range was the widest, between 300kHz and 1MHz. I use it for all pathologies: lumbago, muscular and tendon problems, joint stiffness... I can't do without it anymore. On a daily basis, I would say that I do about ten treatments a day with it. I talk about it around me, and I sometimes present it to colleagues. It's a great machine, which brings a plus to our daily life, which makes us more efficient."
Sports physiotherapist, France
“Using ice to treat an inflammation is essential in traumatology as well as for recovery purposes. What’s more, the mobility inherent to our sport makes the ice treatment difficult to use. But Winshock answered all of our team’s expectations in this field. At the time of the Catalogna Tour, our leader Thibaut Pinot (the 3 big Tours stage race winner, who came 3rd in the 2014 Tour de France, and won the 2018 Lombardie Tour…) was treated using this new technology in order to maximise his recovery when facing the extreme demands of the mountain stages”
Physiotherapist of Groupama-FDJ cycling team, France
"Many triathletes know about tecar therapy and are asking for this type of care. The Winback tecar therapy fits perfectly into this kind of event because it leaves the physio's hands free to practice his art (manual therapy or massage). Combined with other physiotherapy techniques (joint mobilisation, stretching, dry needling, neuro-muscular taping), it is a valuable aid to the success of my treatments."
Physiotherapist specialising in sports pathology, in charge of Ironman triathletes, France
"Winback has become our "Swiss Army Knife" of modalities. The attachments offer endless applications, patients feel the difference and it gets the job done. Winback is comfortable, gentle and rapidly improves mobility. Acute patients find it soothing while patients with chronic musculoskeletal conditions find the increased mobility and reduced pain welcomed. Athletes find it useful for recovery enabling greater intensity in training."
Chiropractic influencer and educator, Chief of Chiropractic services at DeFabio Spine and Sports Rehab, Berkeley Heights, NJ, USA
"I was able to work with Winback to develop the Hi-TENS by R-Shock device and the results are amazing: The pain management immediately makes the horses attentive and cuddly, whereas they were fearful and aggressive. The beneficial effect on behaviour lasts for several weeks after the session, the owners tell me. Hi-TENS is for me the natural and much more effective alternative to infiltrations."
Veterinarian, Osteopath, Acupuncturist & Expert at the Court of Appeal of Rennes, Le Palais, France
“It is the efficiency of the Winback technology in the drainage which has seduced me most. The FixPads allow me to keep the freedom of my hands and to keep my gestures with the power of teech therapy in addition.”
Massage and physiotherapist, France
"Since we use the Winback device, we can provide our patients fast and efficient help. The results are unbeatable: Only 2-3 sessions are necessary for patients between the ages of 50 and 87 suffering from arthrosis, back and joint pain, as well as dystrophic tissue alterations, to achieve permanent pain relief.“
VeritasMed GmbH, Frankfurt, Germany
"The Winback therapy is now part of my daily routine, it complements and reinforces my manual work. Its modularity allows me to adapt it to any type of treatment, from the very fine rehabilitation of the hand to the thigh of the high level sportsman. I particularly appreciate the bracelets which allow me to treat with Winback energy with great precision and the immediate feeling of tissue modifications."
Sport physiotherapist, France
“The frequency range developed by WINBACK allows precise targeting of different tissue layers (muscles, joints, bones, etc.), working on deep-set and painful conditions which were previously unresponsive.”
Chiropractor, Orange, CA, USA
Winback Academy International Committee
"Thanks to the versatility of Winback technologies, I can enhance my physio-aesthetic method and express my holistic approach."
Physiotherapist, Hydrokinesitherapist & Wellness
Specialist, Terlizzi, Italy
Winback Academy International Committee
"Winback is a healing and human movement company which offers a remarkable and affordable tissue recovery and pain management solution. Rehab starts with Winback!”
Physical Therapist, Director Ambulatory Rehabilitation Therapy Services, Johns Hopkins Hospital, Baltimore, MD, USA
Winback Academy International Committee
"Winback is the only technology that allows me to combine manual therapy and technology to optimize mobility, analgesia and trophicity. Winback is an extension of my hands!"
Physical Therapist, Endocrine Dysfunctions
& Women’s Health Specialist, Paris, France
Winback Academy International Committee
"Winback is the most innovative technology of the last 10 years. The Winback Tecar is the essential technology for both manual therapy and active work."
Physical Therapist and Osteopath specialized in Sport, Paris, France
Winback Academy President
“Do you know a technology that integrates manual therapy, active movement and that improves the healing process and the viscoelasticity of the tissues? I do: Winback”
Physical Therapist, Director of Sport PRO Training Center, Sports & Rehabilitation Specialist, Barcelona, Spain
Winback Academy International Committee
"I have been working with tecartherapy for 18 years from now and feeling how the tissue changes under your hands in a few minutes when I apply it is like magic."
Physical Therapist, Director of TARSO Clinic, Pelvic Floor
Specialist, Almería, Spain
Winback Academy International Committee
"After treatment I can always feel improved pliability, less tension and better quality of movement in structures we are treating."
Chiropractor, Integrated Medical Center, Jupiter, FL, USA
International Committee Winback Academy US
"What sold me on Winback as a massage therapist are bracelets: I can feel the energy through myself and my patients! My Winback TECAR modality amplifies my massage therapy sessions with deep penetrating warmth that encourages soft tissue response to structured touch with intention. My results with clients have accelerated!"
LMT, ATC, Owner at Benny Vaughn Athletic, world renowned sports massage therapist, participated in 5 Olympic games
"Retrouver la mobilité perdue est une priorité dans ma pratique, et je vois comment Winback TECAR m'aide à atteindre cet objectif. "
Chiropractor, President ACA Rehab Council, Los Angeles, CA, USA
Winback Academy International Committee
"I almost halved the number of sessions for the same result. I was immediately blown away, it's really a continuation of the manual work."
Physiotherapist, France
"I’ve found the integration of Winback TECAR therapy into my clinical practice has been seamless and powerful. TECAR doesn’t detract from treatment sessions, and delivers immediate results."
Physical Therapist, CEO RunDNA, Wilmington, DE, USA
Winback Academy International Committee
"What I appreciate most about Winback is the approach constantly aimed at innovation, as well as the high and unparalleled dynamism of their electro-medical systems capable of guaranteeing the best therapeutic result for our patients."
Osteopath and Sport Physio, president of Physio Sport Clinic and 1st Physio of the Olympic Italian Cycling Team, Italy
Winback Academy International Committee
“For me, Hi-TENS by R-SHOCK is undoubtedly a revolutionary technology because it combines low and high frequency very well, almost making two devices in one, with a multitude of applications for the physiotherapist”
Physiotherapist, Spain